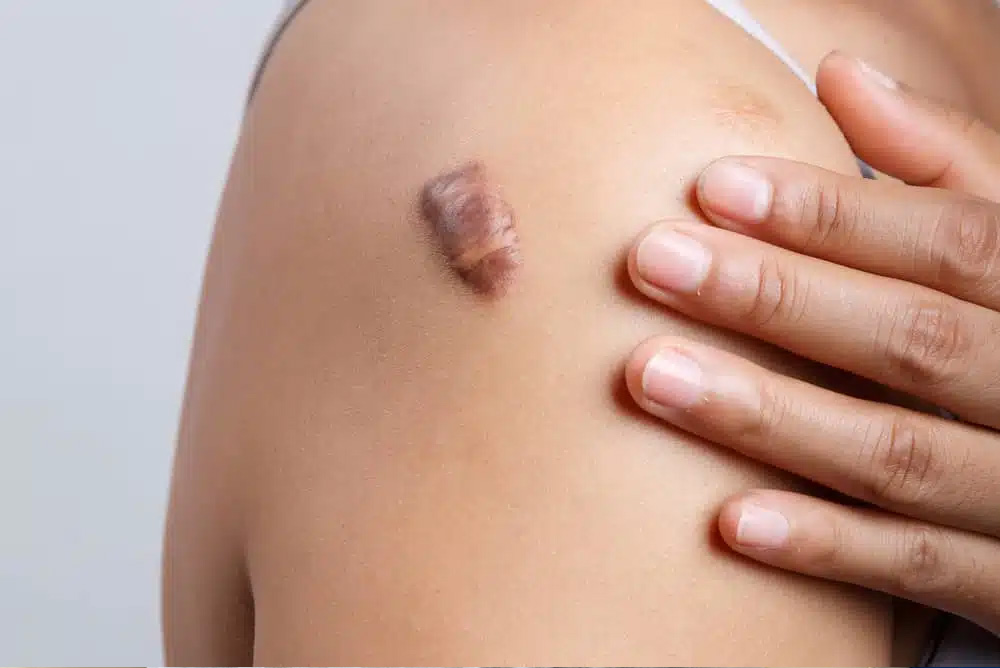
Keloids Explained: Why Some Scars Keep Growing — And What Modern Dermatology Can Do About It.
DR.T.annapurna
ARSHI SKIN AND HAIR CLINICS
Scars are a natural part of healing. But sometimes, the healing process goes into overdrive. Instead of fading, the scar grows thicker, firmer, and extends beyond the original wound. It may itch, hurt, or continue enlarging over years. This condition is called keloid, and it represents one of the most challenging problems in dermatology.
Modern research has significantly improved our understanding of why keloids form and why they are so difficult to treat.
What Exactly Is a Keloid?
A keloid is not just a “big scar.”
It is an abnormal overgrowth of fibrous tissue that:
- Extends beyond the boundaries of the original injury
- Does not regress naturally
- May continue growing for years
- Often causes itching, pain, or discomfort
Unlike hypertrophic scars (which stay within the wound margins), keloids invade surrounding normal skin.
Common sites include:
- Ear lobes
- Chest
- Shoulders
- Upper back
Keloids can sometimes even develop without a clearly remembered injury.
Who Is More Prone to Keloids?
Keloids are more common in:
- Individuals with darker skin tones
- People of African, Asian, or Hispanic origin
- Age group 10–30 years
- Females slightly more than males
Genetics plays a major role. Some families show a strong inheritance pattern, meaning keloids can run in families.
Certain medical conditions such as asthma and atopic disorders may also be associated.
Why Do Keloids Form?
Normally, wound healing occurs in four stages:
- Clot formation
- Inflammation
- Tissue repair
- Remodeling
In keloids, the remodeling stage fails.
Instead of stopping collagen production, the body continues producing excessive collagen — particularly type I and type III collagen — leading to thick, fibrotic overgrowth.
But that is only part of the story.
The Science Behind Keloids –
Modern research shows that keloids are not just “extra collagen.” They involve multiple biological changes.
1. Overactive Fibroblasts
Fibroblasts are cells that produce collagen. In keloids:
- A specific mesenchymal fibroblast subtype increases
- These cells produce excessive extracellular matrix proteins
2. Growth Factors Gone Wild
A key molecule called TGF-β (Transforming Growth Factor Beta) plays a central role.
In keloids:
- TGF-β signaling is overactive
- Fibroblasts become resistant to normal cell death
- Collagen synthesis increases dramatically
3. Immune System Imbalance
Keloid tissue shows:
- Increased inflammatory immune cells
- Higher levels of inflammatory cytokines such as IL-6
- Mast cell activation
This creates a chronic inflammatory microenvironment that keeps stimulating scar growth.
4. Excess Blood Vessel Formation
VEGF (vascular endothelial growth factor) is elevated, promoting abnormal blood vessel growth within the scar.
5. New Discoveries
Recent findings suggest:
- Certain nerve-related cells (Schwann cells) may contribute to fibrosis
- Genetic regulators like microRNAs influence scar formation
All this tells us that keloids are biologically active lesions — not simple scars.
Symptoms Patients Experience
Keloids may cause:
- Persistent itching
- Pain or tenderness
- Burning sensation
- Cosmetic distress
- Restricted movement (if near joints)
Many patients delay treatment due to embarrassment — especially when lesions appear in sensitive areas.
Diagnosis: How Do We Confirm It?
Diagnosis is usually clinical.
We evaluate:
- History of lesion growth beyond original injury
- Progressive enlargement
- Firm rubbery consistency
Dermoscopy may help distinguish keloids from:
- Hypertrophic scars
- Dermatofibroma
- Other fibrous skin lesions
In uncertain cases, biopsy confirms the presence of thick, hyalinized collagen bundles.
Why Are Keloids So Hard to Treat?
Because:
- They have genetic predisposition
- Immune pathways are activated
- Multiple molecular pathways are involved
- Recurrence rates can be high
This is why single treatments often fail.
Modern Treatment Options (Evidence-Based Overview)
1. Intralesional Corticosteroid Injections (Gold Standard)
Triamcinolone acetonide:
- Reduces inflammation
- Suppresses fibroblast proliferation
- Decreases collagen production
Improvement rates are good, especially in smaller or early lesions.
However, possible side effects include:
- Skin thinning
- Visible small blood vessels
- Recurrence
2. PRP (Platelet-Rich Plasma)
Combining PRP with steroid injections:
- Improves wound remodeling
- Reduces recurrence
- Promotes more organized collagen deposition
3. Silicone Gel Sheets
A non-invasive option:
- Hydrates scar
- Modulates fibroblast signaling
- Improves thickness and color
Best suited for early or smaller lesions.
4. Laser Therapy
Options include:
- Pulsed Dye Laser
- Fractional CO₂ laser
- Nd:YAG laser
These help reduce redness, thickness, and improve texture.
5. Cryotherapy (Freezing Therapy)
Cryotherapy involves applying extreme cold (usually liquid nitrogen) directly to the keloid. The freezing process:
- Causes controlled destruction of scar tissue
- Reduces fibroblast activity
- Promotes collagen remodeling
It is particularly useful for smaller or firm keloids, and is often combined with steroid injections for better results. After treatment, the area may blister or temporarily darken before healing. While effective in reducing thickness, multiple sessions are usually required.
6. Surgical Excision
Surgery alone carries a high recurrence rate.
Therefore, it is always combined with:
- Steroid injections
- PRP
- Radiation (in selected cases)
- Silicone therapy
7. Emerging Molecular Treatments
Research is exploring:
- JAK/STAT pathway inhibitors
- TGF-β blockers
- RNA-based therapies
- Monoclonal antibodies
- Stem cell therapy
These are promising but still evolving.
How We Approach Keloids at Arshi Skin and Hair Clinics
At Arshi Clinics, we follow a personalized, combination-based approach, because no single treatment works for everyone.
Step 1: Detailed Assessment
- Size, duration, location
- Symptoms (pain, itching)
- Previous treatments
- Family history
Step 2: Tailored Combination Therapy
Depending on the case:
- Intralesional triamcinolone
- Steroid + PRP combination
- Silicone therapy
- Laser therapy
- Cryotherapy (when indicated)
- Surgical excision with post-procedure protocol
We avoid monotherapy in large or recurrent keloids.
Step 3: Recurrence Prevention
- Scheduled maintenance injections
- Scar modulation protocol
- Lifestyle guidance
- Long-term follow-up
Step 4: Psychological Support
We recognize:
- Emotional impact
- Address Cosmetic concerns
- Help cope Social anxiety.
Our goal is not just scar reduction — but improvement in quality of life.
What Patients Should Understand
- Keloids are not infections.
- They are not cancerous.
- They are genetically influenced.
- Early treatment improves outcomes.
- Combination therapy works better than single treatment.
Most importantly:
Management is a process, not a one-time procedure.
Final Thoughts
Keloids represent a complex interaction between genetics, immune dysregulation, fibroblast overactivity, and molecular signaling pathways.
We now understand more about:
- TGF-β/Smad pathway
- IL-6 and inflammatory signaling
- VEGF-mediated angiogenesis
- Mesenchymal fibroblast activation
Yet recurrence remains a challenge.
The future lies in:
- Targeted molecular therapy
- Personalized medicine
- Combination treatment protocols
At Arshi Skin and Hair Clinics, we integrate scientific evidence with clinical expertise to design individualized treatment strategies that reduce symptoms, improve appearance, and minimize recurrence.
Keloids may be stubborn — but with the right approach, they can be controlled.
If you are struggling with a growing scar, seek early dermatological consultation. The sooner we intervene, the better the outcome.