Dark skin near mouth and nose corners?Understanding seborrheic melanosis
DR.T.Annapurna
ARSHI SKIN AND HAIR CLINICS,Hyderabad
M.B.B.S,DDVL,FRGUHS,MA-PSYCHOLOGY.
Dermatologist,Dermatosurgeon & Aesthetic medicine physician

Facial pigmentation is one of the most common dermatological concerns seen in clinical practice. While conditions like melasma and post-inflammatory hyperpigmentation are widely recognized, seborrheic melanosis is an important but often overlooked cause of facial pigmentation.
Seborrheic melanosis is characterized by brown or greyish pigmentation occurring in oily areas of the face, particularly around the nose, nasolabial folds, mouth corners, eyebrows, and forehead. It commonly develops in individuals with seborrheic dermatitis, oily skin, or chronic inflammation in seborrheic areas.
At Arshi Skin and Hair Clinic, dermatologists frequently diagnose and treat seborrheic melanosis using a root-cause based approach that focuses on controlling seborrheic inflammation, restoring skin barrier health, and safely reducing pigmentation.
This article explains what seborrheic melanosis is, its causes, symptoms, diagnosis, and the most effective treatment options available today.
What is Seborrheic Melanosis?
Seborrheic melanosis is a form of facial hyperpigmentation associated with seborrheic dermatitis or sebaceous gland activity. It typically appears as diffuse brown pigmentation in areas rich in sebaceous glands.
These areas include:
- Around the nose
- Nasolabial folds
- Around corners of mouth,upper part of chin
- Eyebrows
- Glabella (between eyebrows)
- Forehead
- Beard area in men
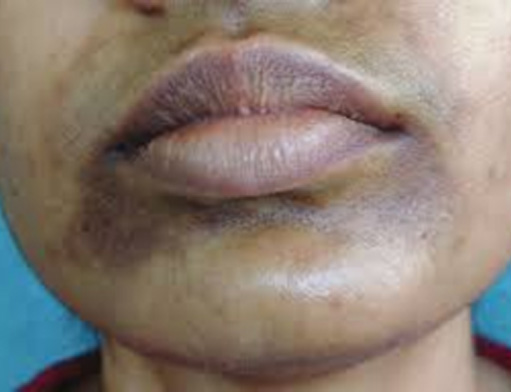
These regions produce higher levels of sebum (oil), making them susceptible to chronic low-grade inflammation and yeast colonization, which can stimulate melanin production.
Over time, persistent inflammation leads to post-inflammatory pigmentation, resulting in visible darkening of the skin.
Causes of Seborrheic Melanosis
Several factors contribute to the development of seborrheic melanosis.
1. Seborrheic Dermatitis
The most common underlying cause is seborrheic dermatitis, a chronic inflammatory skin condition.
It occurs due to:
- Overactive sebaceous glands
- Skin microbiome imbalance
- Yeast overgrowth (Malassezia species)
- Genetic predisposition
Symptoms include:
- Redness
- Greasy skin
- Scaling
- Itching
Persistent inflammation from seborrheic dermatitis stimulates melanocytes (pigment cells), leading to pigmentation.
2. Malassezia Yeast Overgrowth
Malassezia yeast is naturally present on human skin. However, in oily areas it can proliferate excessively and cause:
- Inflammation
- Skin irritation
- Increased pigment production
This contributes significantly to pigmentation around seborrheic areas of the face.
3. Skin Barrier Damage
An impaired skin barrier leads to:
- Increased skin sensitivity
- Chronic irritation
- Inflammatory pigment production
Patients with seborrheic skin often use harsh products that further damage the barrier, worsening pigmentation.
4. Friction and Repeated Rubbing
Frequent touching or rubbing of irritated areas, particularly around the nose or eyebrows, can trigger post-inflammatory hyperpigmentation.
Symptoms of Seborrheic Melanosis
Common symptoms include:
Facial Pigmentation
Brown or greyish discoloration around seborrheic areas.
Oily Skin
Increased oil production in the affected regions.
Mild Scaling
Fine flakes or dandruff-like scaling near eyebrows and nose.
Redness or Irritation
Low-grade inflammation may be present.
Itching
Some patients experience mild itching or discomfort.
Unlike melasma, seborrheic melanosis is localized specifically to seborrheic areas rather than appearing symmetrically across the cheeks.
How Dermatologists Diagnose Seborrheic Melanosis
Diagnosis is mainly clinical but may involve additional dermatological evaluation.
Dermatologists assess:
- Pattern of pigmentation
- Skin oiliness
- Presence of seborrheic dermatitis
- Scaling and redness
Dermoscopy examination often reveals:
- Diffuse brown pigmentation
- Perifollicular pigment pattern
- Background erythema
- Fine scales
Accurate diagnosis is important because treatment differs significantly from melasma or other pigment disorders.
Conditions That Can Mimic Seborrheic Melanosis
Several pigmentation disorders may resemble seborrheic melanosis.
Melasma
Symmetrical pigmentation on cheeks, forehead, and upper lip caused by hormones and sun exposure.
Lichen Planus Pigmentosus
Slate-grey pigmentation often affecting the face and neck.
Pigmented Contact Dermatitis
Pigmentation triggered by cosmetics, perfumes, or hair dyes.
Post-Inflammatory Hyperpigmentation
Occurs after acne or skin injury.
A dermatologist must differentiate between these conditions to provide the correct treatment.
Treatment of Seborrheic Melanosis
Successful treatment requires addressing both inflammation and pigmentation. Simply treating pigmentation without controlling seborrheic dermatitis often results in recurrence.
1. Antifungal Treatment
Since Malassezia plays a major role, dermatologists prescribe topical antifungal medications.
These include:
- Ketoconazole creams
- Ciclopirox formulations
- Sertaconazole creams
These medications help control yeast overgrowth and inflammation.
2. Anti-Inflammatory Therapy
To reduce skin inflammation, dermatologists may prescribe:
- Calcineurin inhibitors (tacrolimus or pimecrolimus)
- Short courses of mild corticosteroids
Reducing inflammation prevents further pigmentation.
3. Depigmenting Agents
Once inflammation is controlled, dermatologists introduce pigment-reducing agents.
These include:
- Azelaic acid
- Kojic acid
- Alpha arbutin
- Niacinamide
- Retinoids
These ingredients help regulate melanin production and gradually lighten pigmentation.
Dermatological Procedures for Seborrheic Melanosis
Chemical Peels
Superficial chemical peels remove pigmented skin cells and stimulate regeneration.
Common peels include:
- Glycolic acid peel
- Mandelic acid peel
- Lactic acid peel
- Salicylic acid peel
These treatments improve skin texture, oil control, and pigmentation.
Laser Treatment for Pigmentation
Advanced dermatology clinics may use laser therapy to treat resistant pigmentation.
Common technologies include:
- Q-switched lasers
- Laser toning
- Low-fluence pigment lasers
Lasers break down excess pigment and stimulate skin renewal. However, they must be used cautiously in darker skin types to avoid complications.
Seborrheic Melanosis Treatment at Arshi Skin and Hair Clinics
At Arshi Skin and Hair Clinic, seborrheic melanosis is treated using a scientific dermatology protocol that focuses on long-term skin health.
1. Accurate Diagnosis
Dermatologists perform detailed clinical examination and dermoscopic analysis to confirm seborrheic melanosis and rule out other pigmentation disorders.
2. Seborrheic Control Therapy
Treatment begins by controlling seborrheic dermatitis using:
- Antifungal medications
- Anti-inflammatory therapy
- Oil regulation protocols
This prevents further pigment formation.
3. Skin Barrier Restoration
Customized skincare regimens are prescribed to repair the skin barrier.
- Ceramide moisturizers
- Gentle cleansers
- Anti-inflammatory active ingredients
Barrier repair reduces irritation and recurrence.
4. Advanced Pigment Reduction Treatments
Once inflammation is controlled, dermatologists may recommend:
- Medical depigmenting treatments
- Customized chemical peels
- Advanced laser therapies when required
This staged approach ensures safe, gradual, and effective pigmentation reduction.
laser treatment in hyderabad
chemical peel treatment in hyderabad
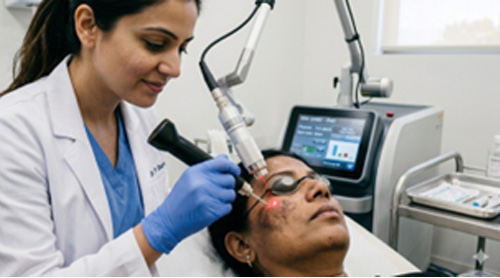
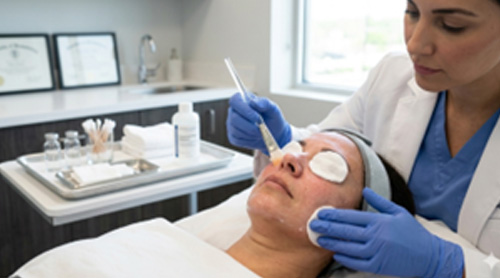
How to Prevent Seborrheic Melanosis
Prevention plays an important role in long-term management.
Dermatologists recommend:
Maintain Gentle Skincare
Avoid harsh soaps and aggressive scrubbing.
Control Seborrheic Dermatitis Early
Treat dandruff and facial scaling promptly.
Use Sunscreen Daily
Sun exposure can worsen pigmentation.
Avoid Irritating Cosmetics
Choose non-comedogenic and fragrance-free products.
When to See a Dermatologist
Consult a dermatologist if you notice:
- Persistent pigmentation around the nose or eyebrows
- Oily skin with scaling and discoloration
- Pigmentation not improving with regular skincare
Early treatment can prevent pigmentation from becoming more persistent.
Conclusion
Seborrheic melanosis is an often underdiagnosed cause of facial pigmentation, typically associated with seborrheic dermatitis and chronic inflammation in oily areas of the face. Because it can resemble other pigment disorders, accurate diagnosis by a dermatologist is essential.
Effective treatment requires a comprehensive approach that addresses inflammation, skin barrier dysfunction, and pigment production.
At Arshi Skin and Hair Clinics,located in gachibowli,madinaguda,hitec city,nallagandla,and banjara hills in hyderabad, patients receive personalized dermatological care using evidence-based treatments, advanced procedures, and holistic skin management strategies. This ensures safer treatment outcomes and long-term improvement in skin clarity and health.
If you are experiencing persistent facial pigmentation around seborrheic areas, consulting an experienced dermatologist can help identify the underlying cause and provide the most effective treatment plan.


